Brain adaptability, often described as the brain’s ability to adapt its structure and function in response to experience, learning, or neurological damage, represents a fundamental principle in modern clinical science. For many years, scientists assumed that the human brain stopped developing after childhood. However, ongoing research has confirmed that the brain continues to form additional neural pathways throughout adulthood. This dynamic feature allows the nervous system to reorganize itself after injury caused by stroke, traumatic brain injury, or neurological disorders. Recognizing neuroplasticity has become a central focus in rehabilitation medicine because it provides a evidence-based framework for recovery and observable progress.
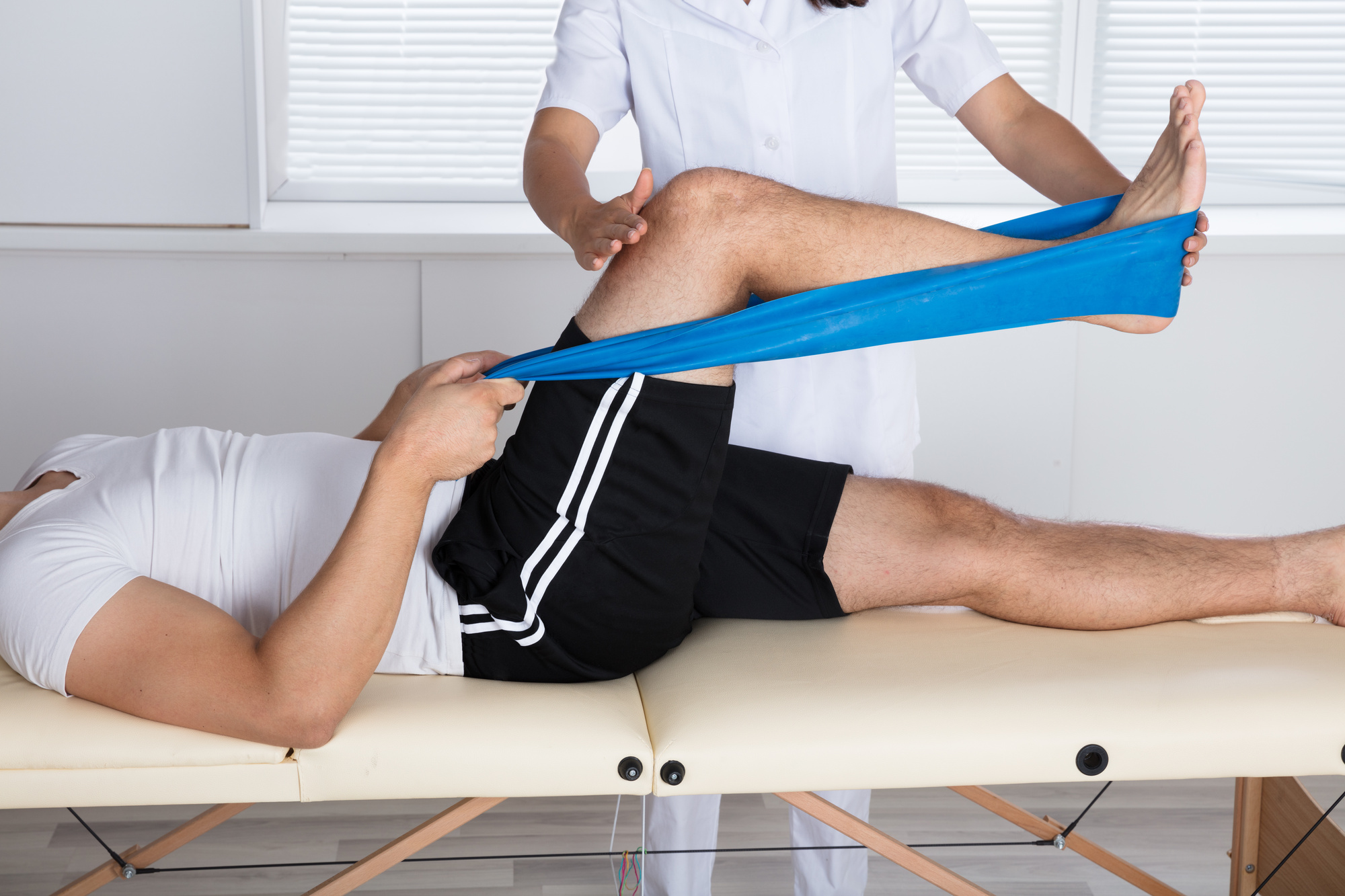
When an insult affects the brain or neural structures, certain neural connections may be disrupted or lost. Through structured therapy and repeated training, alternative synaptic connections can emerge to offset damaged areas. This mechanism is known as neural reorganization. Clinical practitioners use evidence-based treatment strategies such as physical therapy, occupational therapy, and speech-language therapy to stimulate this restorative process. Structured repetition, goal-directed exercises, and motor learning principles are essential components that promote the formation of more efficient brain pathways. Over time, consistent clinical training can improve movement ability, cognitive function, balance, coordination, and speech function.
The concept of neural flexibility also plays an significant part in neurocognitive therapy. Individuals healing after conditions such as brain injury or traumatic brain injury may experience challenges with memory, focus, and executive functioning. Structured mental exercises are developed to strengthen higher-level thinking a fantastic read skills and cognitive processing through systematic brain-based activities. Activities that involve attention control, working memory tasks, and analytical techniques help activate underused areas of the cerebral cortex. As these brain networks are repeatedly engaged, they become more efficient, supporting steady progress in daily functioning and independence.
In addition to conventional therapies, advanced clinical technologies are enhancing the implementation of neuroplasticity principles in clinical environments. Immersive digital platforms, robotic-assisted therapy, and neuromodulation techniques such as targeted magnetic stimulation are being incorporated into treatment plans. These advanced tools provide precise, measurable, and interactive ways to deliver structured therapy. For example, robotic devices can support limb movement to strengthen correct motor patterns, while virtual environments simulate functional tasks that support skill restoration. Such innovations increase patient motivation and provide valuable feedback, which further supports adaptive change.
The expanding knowledge of brain adaptability has reshaped how Learn More Here healthcare professionals approach rehabilitation. Rather than emphasizing solely adjusting to lost abilities, rehabilitation now emphasizes restoring function through active engagement and intentional training. Early intervention, personalized care strategies, and active involvement are critical factors in achieving successful results. By applying the science of brain plasticity, clinicians can design recovery methods that are based on clinical evidence and supported by measurable progress. This shift in clinical approach offers renewed hope for individuals facing neurological challenges and highlights the brain’s proven ability for functional change and growth.